Why Healthcare Workforce Planning Must Move Beyond Vacancy Rates and Open Reqs
Vacancy rates and open requisitions matter. They tell leaders where the hiring queue is backing up and where labor costs will likely rise next. But they are weak proxies for whether a health system can actually deliver care safely, consistently, and at the level of complexity its patients now require. In U.S. healthcare, the problem is no longer just “How many openings do we have?” The harder question is “Where are our critical capabilities thin, fragile, or missing?” Recent federal projections show why this matters: HRSA continues to project meaningful shortages across parts of the nursing workforce, primary care, and behavioral health, with especially acute pressure in nonmetro areas and in several behavioral health professions. At the same time, the 2024 national nursing workforce survey found that more than 138,000 nurses left the workforce since 2022 and that almost 40% intend to leave by 2029. Those are not just staffing problems. They are signals of capability risk. (Health Resources and Services Administration [HRSA], 2025a, 2025b, 2025c; Smiley et al., 2025).
A vacancy-based view also misses an important point: healthcare outcomes depend on more than headcount in a few heavily measured roles. A 2024 qualitative study in BMC Health Services Research found that patient outcomes are shaped not only by registered nurse staffing, but also by the mix of interprofessional team members, hospital context, and community resource constraints. A 2025 systematic literature review similarly argued that health workforce planning needs to move from a “professional-centric” model to a more “job-centric” model that reflects new care models, data realities, and competency needs. In plain English, that means leaders should plan for what work must get done, which capabilities are required to do it well, and how long those capabilities take to build, not just how many openings sit in the applicant tracking system. (Gabutti et al., 2025; Ziemek et al., 2024).
This shift matters because capability gaps show up operationally long before they show up on a vacancy report. They appear as overloaded charge nurses, delayed discharge planning, thin behavioral health coverage, poor preceptor capacity for new graduates, weak manager follow-through, or teams that cannot use digital tools well enough to reduce documentation burden. These gaps affect access, throughput, quality, safety, and retention at the same time. In a 2024 meta-analysis in JAMA Network Open, nurse burnout was associated with lower healthcare quality and safety and lower patient satisfaction. The American Hospital Association’s 2025 workforce scan also notes that many organizations remain concerned about new clinical graduates’ readiness for bedside care and are responding with extended orientation, preceptors, residencies, and more deliberate workload balancing. That is exactly the point: the issue is not only whether a role is filled, but whether the organization has enough experienced, supported, and deployment-ready capability behind the role. (American Hospital Association [AHA], 2024; Li et al., 2024).
A better planning model starts with four questions. First, which capabilities are most critical to care delivery, access, safety, and margin in the next 12 to 24 months? Second, where is the current bench shallow or unstable? Third, how long would it take to close the gap through hiring, internal development, redesign, or automation? Fourth, what is the business and patient-risk exposure if the gap remains open? That approach creates a much more useful planning conversation than vacancy counts alone. It moves leaders from reactive staffing to strategic capacity design. (Gabutti et al., 2025; HRSA, 2025a).
Below is an illustrative healthcare capability heatmap for a U.S. health system. It is not meant to represent any one organization’s actual data. It shows the kind of view leadership teams should build using their own workforce, quality, access, finance, and experience data.
Illustrative healthcare capability heatmap
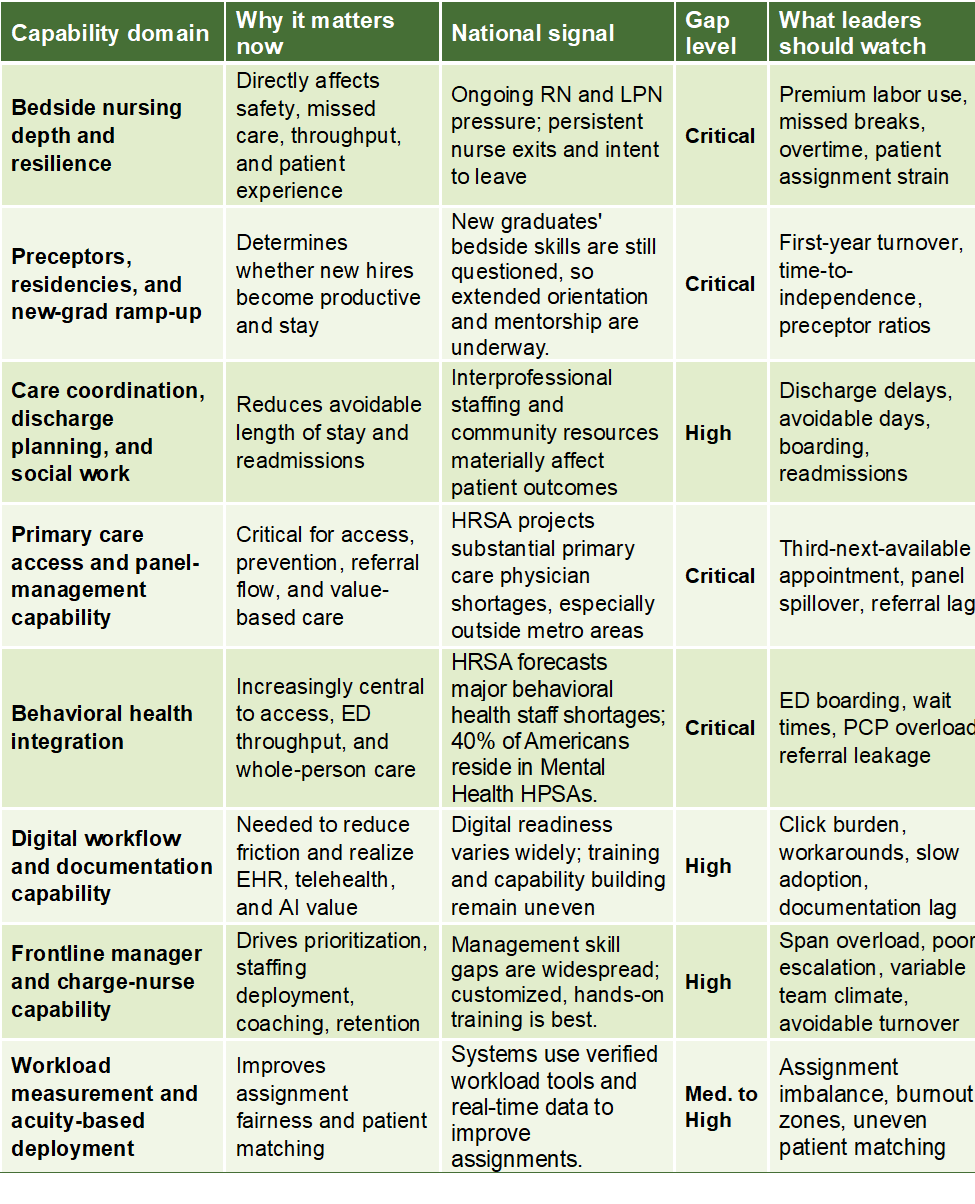
Heatmap note: The ratings above reflect current evidence on shortages, interprofessional staffing needs, graduate readiness, digital capability, and management capability. Your version should replace the ratings with internal data and trend lines. (AHA, 2024; Alotaibi et al., 2025; Gabutti et al., 2025; Giovanelli et al., 2024; HRSA, 2025b, 2025c; Smiley et al., 2025; Ziemek et al., 2024).
Two capabilities deserve special attention in 2026. The first is digital workflow capability. Many organizations talk about EHR optimization, ambient documentation, AI decision support, or digital front doors as technology initiatives. In practice, they are workforce capability initiatives. A 2025 systematic review found that digital readiness and capability among healthcare professionals depends on targeted interventions, role-relevant learning, and the removal of barriers that impede adoption. If leaders plan technology but do not plan for digital capability, they will mistake implementation for transformation. (Alotaibi et al., 2025).
The second is frontline manager capability. Health systems often promote technically strong clinicians into management roles and then assume experience will substitute for management preparation. Recent research suggests that assumption is costly. A 2024 study on management training in healthcare found that effectiveness improves when training is tailored to participant profiles, uses varied pedagogical approaches, and addresses actual competency gaps rather than delivering generic content. In operational terms, that means manager capability should appear on the workforce heatmap just as clearly as RN supply or physician access. Weak frontline management magnifies turnover, inconsistency, and burnout. Strong frontline management improves deployment, coaching, learning transfer, and team stability. (Giovanelli et al., 2024).
So what should a leadership team do next? Start by rebuilding workforce planning around capabilities, critical roles, and time-to-readiness. Use vacancies and reqs as supporting indicators, not the centerpiece. Build a capability heatmap for the next 12 to 24 months. Include at least five data families: staffing and vacancy data, retention and tenure patterns, access and throughput measures, quality and safety measures, and learning or readiness indicators such as time-to-proficiency and preceptor capacity. Then ask three hard questions every month: Where are we one departure away from operational fragility? Which gaps can we solve through development or redesign rather than pure hiring? Which capability gaps pose the greatest risk to patient access, safety, and margin if we do nothing? That is how workforce planning becomes a strategic instrument instead of a recruiting report. (Gabutti et al., 2025; HRSA, 2025a; Ziemek et al., 2024).
Healthcare organizations do still need better recruiting. But recruiting alone will not solve structural fragility in nursing, primary care, behavioral health, digital adoption, or frontline management. The organizations that outperform over the next several years will be the ones that can see capability risk earlier, develop talent faster, redesign work more intelligently, and match scarce expertise to the work that matters most. Vacancy rates tell you who is missing. A capability heatmap tells you what is vulnerable. Leaders need both, but they should not confuse one for the other. (AHA, 2024; HRSA, 2025a, 2025b, 2025c).
To get a copy of a full capabilities heat map, please let me know.
References
Alotaibi, N., Brown Wilson, C., & Traynor, M. (2025). Enhancing digital readiness and capability in healthcare: A systematic review of interventions, barriers, and facilitators. BMC Health Services Research, 25, 500. doi:10.1186/s12913-025-12663-3
American Hospital Association. (2024). 2025 health care workforce scan.
Gabutti, I., Pandolfi, D., Apuzzo, L., & Martini, L. (2025). Health workforce planning in the era of proximity healthcare: A systematic literature review. Health Services Management Research. Advance online publication. doi:10.1177/09514848251398797
Giovanelli, L., Rotondo, F., & Fadda, N. (2024). Management training programs in healthcare: Effectiveness factors, challenges and outcomes. BMC Health Services Research, 24, 904. doi:10.1186/s12913-024-11229-z
Health Resources and Services Administration. (2025a). State of the U.S. health care workforce, 2025.
Health Resources and Services Administration. (2025b). State of the primary care workforce, 2025.
Health Resources and Services Administration. (2025c). State of the behavioral health workforce, 2025.
Li, L. Z., Yang, P., Singer, S. J., Pfeffer, J., Mathur, M. B., & Shanafelt, T. (2024). Nurse burnout and patient safety, satisfaction, and quality of care: A systematic review and meta-analysis. JAMA Network Open, 7(11), e2443059. doi:10.1001/jamanetworkopen.2024.43059
Smiley, R. A., Kaminski-Ozturk, N., Reid, M., Burwell, P. M., Oliveira, C. M., Shobo, Y., Allgeyer, R. L., Zhong, E., O’Hara, C., Volk, A., & Martin, B. (2025). The 2024 National Nursing Workforce Survey. Journal of Nursing Regulation, 16(1), S1-S88.
Ziemek, J., Hoge, N., Woodward, K. F., Doerfler, E., Bradywood, A., Pletcher, A., Flaxman, A. D., & Iribarren, S. J. (2024). Hospital personnel perspectives on factors influencing acute care patient outcomes: A qualitative approach to model refinement. BMC Health Services Research, 24, 805. doi:10.1186/s12913-024-11271-x